Motley Talk about John
A man of many talents, from sedating Queen Victoria to saving thousands of lives.
Dear friends, unlike George Johann Scharf from my last article, Dr John Snow (1813 to 1858) was famous, and his gravestone is in the posh west side of Brompton Cemetery. Nowadays he is known for his role in understanding how cholera is transmitted and is considered a founding father of epidemiology. Though in his lifetime he was more famous for being one of the first anaesthetists.
While studying and working at Westminster Hospital Dr Snow became interested in anaesthetics, at the time a very new area of medicine. In particular he studied chloroform. Dr Snow published his research into adjusting the amount of chloroform for each patient, to render the patient insensible so they had little sensation of pain, but not become unconsciousness. Without modern ways of monitoring vital signs, if a patient’s respiration became too shallow they could easily die.
The use of chloroform in childbirth was controversial. Queen Victoria, who hated childbirth (she was not much more enamoured of small babies), was given chloroform by Dr Snow for the births of the last two of her children (in 1853 and 1857). This led to a wider acceptance of obstetrical anaesthesia.

Epidemics have been well known throughout history. We are fortunate to live in a time when modern medicine can hopefully discern the organism causing the disease and understand how to treat it. If you lived during the 19th Century cholera epidemics in London, you would not have been so fortunate. At the time physicians still believed in the miasma theory. From the time of Ancient Greece (miasma is the Ancient Greek work for pollution) until the middle of the 19th century, it was believed that ‘bad air’ carried infectious diseases from polluted or rotting organic matter.

Cholera had been known in the Indian subcontinent for thousands of years. But the first the British heard of it was in 1781, when British soldiers stationed in India became sick; it became the leading cause of death amongst British troops in India. The first incidence of cholera in England occurred in Sunderland in October 1831, when a ship carrying sailors who had the disease docked at the port.
Vibrio cholerae bacterium thrives in excrement. Human waste has always been carefully managed by mankind. But in the 19th Century, the thousands of people flocking to London for work caused problems. London was in effect a medieval city coping with thousands of new residents, but without an effective sewage system, or even a properly managed water source. This allowed cholera-infected human waste to contaminate drinking water, so the cholera was transferred to humans when they drank the water. Within 24 hours of drinking infected water, a perfectly healthy person could be dead. The disease was not understood, the miasma theory the most prevalent, and treatment ineffectual.
Dr Snow studied outbreaks of cholera over many years, and became convinced the infection was waterborne, but he was not believed by the medical establishment. Then, in 1854, there was a large cholera outbreak in Broad Street, Soho, near his home.
Dr Snow was helped by Dr William Farr, who became the first person to track statistics and use them to improve public health. Dr Farr was sceptical about the theory of waterborne cholera, but as well as tracking the age and sex of cholera victims he added information about where they got their drinking water.
This enabled Dr Snow to map cholera victims who used the same water, and he found out that everyone who had become sick in Soho had drunk from the same Broad Street water pump. Some outliers convinced Dr Snow that the Broad Street pump was the source of the infection. One was that none of the 535 people in the St. James Workhouse had died, though it was very close to the Broad Street pump. This was because the workhouse had a private water supply from another supplier, and a well on the premises.
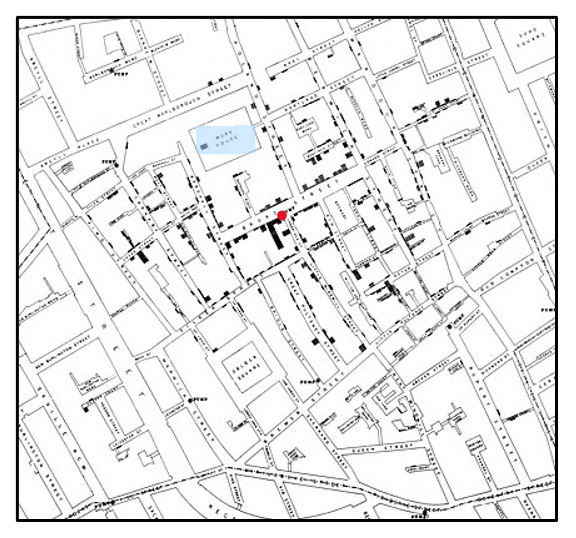
Dr Snow worked tirelessly to gather this data. His friend1 wrote: “no one but those who knew him intimately can conceive how he laboured, at what cost, and at what risk. Wherever cholera was visitant, there was he in the midst.”
Dr Snow was sure the Broad Street pump water was the source of the cholera outbreak and persuaded the board of the St. James Parish to remove the handle of the pump, to stop it being used. In 1855 a young curate, Rev. Henry Whitehead, helped to prove that the Broad Street pump was contaminated.
Rev. Whitehead found out that just before the epidemic a baby had died of cholera, though nobody knew the diagnosis at the time. The Lewis family lived close to the Broad Street pump. Baby Lewis’s nappies (infected with cholera) were seeped in pails of water that were then dumped into the cesspool that lay in the basement of the house. Rev. Whitehead persuaded the authorities to undertake a widespread excavation of the pump and cesspool. They found that the cesspool walls were old and broken, so the contents had seeped into the Broad Street pump water.
Ironically, while water plays host to the cholera bacterium, it is also the cure for the devastating dehydration caused by the disease. At Broad Street victims of the epidemic had used other cesspools or ways of disposing of their waste, so the water at the Broad Street pump had not been reinfected. After the initial infection, when many people died, people who later drank the pump water mostly recovered, because the water was clear of cholera bacteria by then, so it rehydrated them. But the later recovery of patients who had drunk a lot of water from the ‘infected’ pump undermined the waterborne theory.
After the cholera epidemic had subsided, government officials replaced the Broad Street pump handle and rejected Dr Snow’s hypothesis. It was not until 1883 that international recognition was given for the identification and growth of vibrio cholerae bacterium in water.
Sadly, Dr Snow died of a heart attack in June 1858. He was only 45 years old. Some of his friends wondered if his experiments inhaling experimental anaesthetics hastened his end. His first obituary did not even mention cholera. Dr Farr died in 1883 and is regarded as one of the founders of medical statistics. Rev. Whitehead moved to the north of England and died in 1896.
I went to visit the Broad Street pump, and to remember the nearly 500 men, women and children who died within 250 yards of the pump, in a period of less than two weeks.
It is over 150 years later, the street is now called Broadwick Street, the area is no longer poor or run down, and the pump is a replica. But it was poignant to think of all the souls who had died, and of the man who prevented many more people from dying of cholera in the future2. The building of huge sewers in the 1860s, which managed waste effectively, meant the last outbreak of cholera in London was in 1866.
As always, any links are provided to give the reader more information. I do not make any money from these links. Where possible permissions have been sought for the use of images and text, unless they are in the Public Domain. If there is an issue with copyright please contact me.
Benjamin Ward Richardson, friend and biographer.
Sadly, cholera is still a deadly disease in many developing nations.